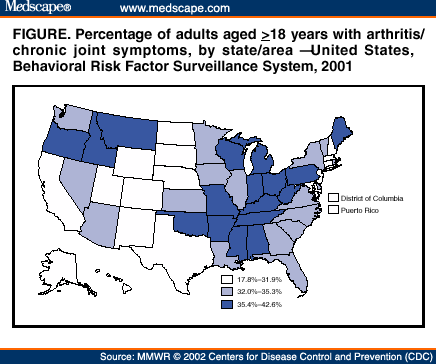
In 2001, questions about arthritis and CJS were asked of adult respondents in every state through the Behavioral Risk Factor Surveillance System (BRFSS).
This estimated U.S. prevalence of arthritis/CJS was 33.0% among adults. Increased intervention efforts, including early diagnosis and appropriate clinical and self-management (e.g., physical activity, education, and maintaining appropriate weight), are needed to reduce the impact of arthritis and CJS.
Respondents were classified as having CJS if they answered "yes" to two questions: "In the past 12 months, have you had pain, aching, stiffness, or swelling in or around a joint?" and "Were these symptoms present on most days for at least a month?" Respondents were considered to have physician-diagnosed arthritis if they answered "yes" to the question, "Have you ever been told by a doctor that you have arthritis?" Respondents reporting either CJS or physician-diagnosed arthritis were classified as having arthritis/CJS. Respondents who did not know, were not sure, or refused to answer were classified as not having either condition. The median response rate for 2001 was 51.4%. Data were weighted by age and sex to reflect each state's most recent adult population estimate.
In 2001, the estimated prevalence of arthritis/CJS among U.S. adults was 33.0% (95% CI=32.7%-33.4%), representing approximately 69.9 million adults (Table 1), including 10.6% (22.4 million) of the adult population with physician-diagnosed arthritis only, 10.0% (20.9 million) with CJS only, and 12.4% (26.6 million) with both. Prevalence increased with age. Women had higher prevalence than men, and non-Hispanic whites and non-Hispanic blacks had higher prevalence than Hispanics and persons of other racial/ethnic groups. Other groups with higher prevalence were persons who had not completed high school, those who were physically inactive, and those who were obese or overweight (i.e., having a body mass index >/=25.0). The median state prevalence was 33.1% (range: 17.8% [Hawaii]-42.6% [West Virginia]) (Table 2), with states in the central and northwestern United States having the highest prevalence (Figure). To reflect each state's burden of arthritis/CJS more accurately, state estimates were made without any adjustment; comparisons among states would require adjusting for recognized risk factors such as age, which differ among states.
Reported by:J Bolen, PhD, CG Helmick, MD, JJ Sacks, MD, G Langmaid, Div of Adult and Community Health, National Center for Chronic Disease Prevention and Health Promotion, CDC.
The findings in this report provide the first direct measurements of arthritis/CJS prevalence for all states. Self-reports are required to estimate prevalence in the population because many persons with arthritis/CJS do not see a clinician for their symptoms, and their conditions remain undiagnosed.[5] Methods to capture self-reported arthritis at the national and state levels have evolved over time. An earlier definition of arthritis based on the International Classification of Diseases, Ninth Clinical Modification (ICD-9-CM) was used to generate the previous national estimate of 43 million (6) and to develop indirect, synthetic state estimates for 1990 by using age-, race/ethnicity-, and region-specific rates.[7]
Since 1996, a different set of self-report questions, developed in part
by the National Arthritis Data Workgroup and not ICD-9-CM-based, has been
used in BRFSS in selected states. The 2001 BRFSS estimate of 69.9 million
persons with arthritis/CJS is considerably higher than earlier estimates,
most likely because of differing case definitions, and does not
indicate a substantial increase in arthritis and CJS prevalence.
The findings in this report are subject to at least five limitations. First, the estimates used self-reported data that were not confirmed by a physician. Second, the sample is drawn from the civilian, noninstitutionalized adult population and does not include military personnel and institutionalized persons. Third, BRFSS is a telephone survey and does not include persons who do not have telephone service. Fourth, the median response rate for 2001 was 51.4%; however, the distribution of demographic characteristics in the BRFSS sample was very similar to the distribution based on U.S. census data (i.e., sex, age, and race data). Finally, whereas previous estimates might have underestimated arthritis/CJS prevalence, BRFSS might overestimate prevalence because it might include persons with injuries rather than arthritis as the cause of CJS (CDC, unpublished data, 2001).
The questions used to define CJS and physician-diagnosed arthritis were modified for the 2002 BRFSS survey. As a result, these prevalence estimates might vary from the 2001 estimates. In 2002, the National Health Interview Survey began using these same case-defining questions; this change will allow better comparisons of national and state prevalence estimates.
BRFSS state-specific estimates of arthritis/CJS are important for planning
and evaluating prevention programs and measuring progress toward meeting
state and national health objectives for 2010. The CDC Arthritis Program
funds arthritis programs in 36 states that rely on these data. These programs
encourage interventions to reduce the impact of arthritis and CJS in state
populations, including early detection and appropriate management of arthritis/CJS.
Interventions include physical activity
programs (e.g., the Arthritis Foundation's PACE [People with Arthritis
Can Exercise] or Aquatics programs) and educational programs (e.g., the
Arthritis Self-Help Course, which has helped persons with arthritis and
CJS experience less pain and reduce the number of clinical visits they
make).[8] Additional information about these programs is available at http://www.arthritis.org/events/getinvolved/programs_services.asp.